Crissy Voigtmann received her Doctor of Physical Therapy from the University of St. Augustine in 2014. She’s a board certified neurologic clinical specialist. She works as a full-time clinician serving patients with brain injury, stroke, neuro oncology, and incomplete spinal cord injury, and spearheads program development for locomotor training for all neurologic patients in the inpatient rehab setting at Orlando Health’s Institute for Advanced Rehabilitation.
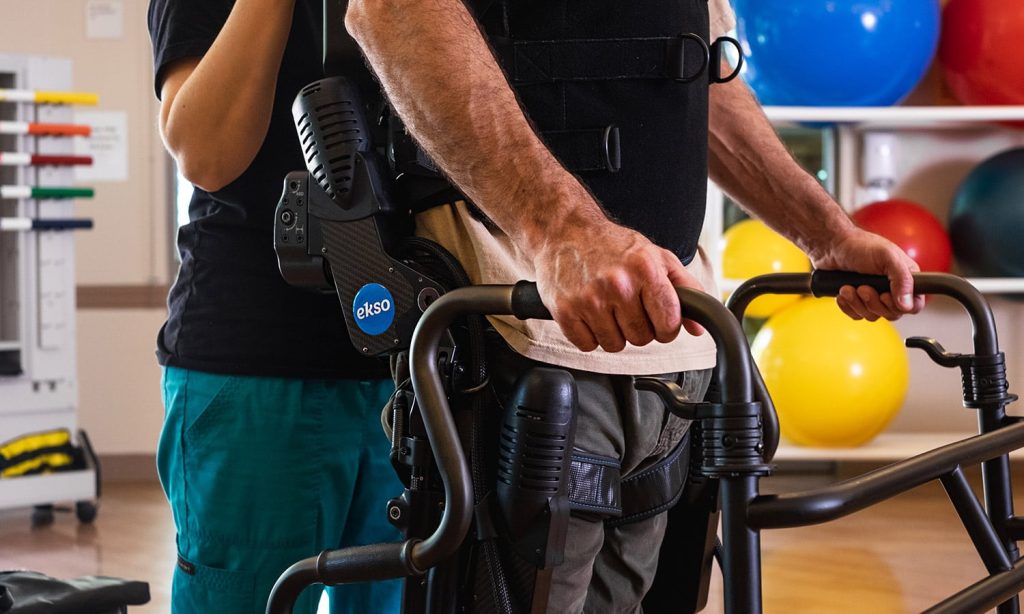
What were the first steps toward introducing EksoNR in a rehab program?
When the doctors at Orlando Health first got the exoskeleton, they were collaborating and came up with this idea of having a lead locomotor person. Dr. Voigtmann became the lead person just to help bridge the gap between their non-Ekso therapists on the floor, with either pairing them with an Ekso therapist or with Dr. Voigtmann herself. They were afforded that ability just by creating the role of lead locomotor therapist at the clinic.
The other first step was a designated area off to the side of the gym, so that the exoskeleton has everything there that it needs. There you will find all evaluation forms and data collection sheets and the measuring tools. Everything is in one spot, so that if someone thinks, “This is a great patient for Ekso. I want to do quick measurements,” the opportunity is available to them. They get that patient on the mat, take the measurements, and that allows them the opportunity to get the patient into the Ekso the next session if the current session is unavailable. They have found that it is a nice way to keep everything in one place.
How do you refer patients to EksoNR?
They tried to come up with a referral system. For example, their unit has nine teams, so nine teams of PT/OT and they only have four Ekso-trained therapists. What do they do with the other teams? They paired up with an Ekso clinician in order to have the opportunity to propose, “Can we switch this patient off? You see one of mine and I’ll see one of yours.” With this method, they could optimize the number of patients getting into the exoskeleton and get the benefits of early gait training.
What else has helped EksoNR be successful in inpatient rehab?
At IFR, they have been very fortunate to have really engaged rehab aides in their unit. They went through training sessions with them on how to do wrenching techniques, how to size the Ekso, how to clean it, and even sometimes how to write down some of the data on a data collection sheet for them if time is critical.
They have been essential in the setup, the breakdown, and taking all of the information. They’re also really skilled at using the Ekso controller so that they don’t have to pull in too many more people. Essentially, there would be a physical therapist who is Ekso-certified and then a tech for each session. That really helps to make it effective; cost efficient for the company, and also time efficient.
Stay Tuned For More Blogs About EksoNR or Click Here to View The Webinar in Full
Who are the candidates for Ekso?
The stroke patients primarily receiving early Ekso intervention:
- Dense Hemiparesis: 0-⅖ MMT throughout affected lower extremity
- Pusher Syndrome
- Significant Postural Control and Awareness deficits
- Motor planning and Sequencing deficits
Other patient specific factors leading to early Ekso utilization:
- Obesity/Height (under 220lbs, under 6’5” approximately)
- Impulsivity
- Cognitive deficits
The overall message is these patients are individuals who are very difficult to manually facilitate. They are very difficult to provide the manual techniques that are necessary to hit high repetitions or to hit high intensity levels. As a result, they are going into the exoskeleton.
Stay Tuned For More Blogs About EksoNR or Click Here to View The Webinar in Full